
If you knew you could change your lifestyle and diet and avoid heart disease and other things, you should do it.
Laila Ali
Each year, more than 800,000 people in the U.S. die from cardiovascular disease. This figure accounts for a whopping percentage of fatalities, making up one in three deaths. To put it into perspective, cardiovascular disease collectively claims more lives than all cancers, diabetes, Alzheimer’s disease, or accidents. As many as 2,200 Americans die of cardiovascular disease each day, with one death occurring every 39 seconds. Cardiovascular disease, the umbrella term referring to all types of diseases affecting the heart or blood vessels, encompasses coronary heart disease and stroke. Alarmingly, more than 10% of Americans have already been diagnosed with heart disease.[1]Despite these grim statistics, there’s still tremendous hope for today’s adult population: heart attack and stroke are largely preventable. To prevent these diseases effectively, however, you must first be able to recognize the warning signs. Browse through this guide as we review some of the most critical information about the life-saving power of heart disease and stroke prevention.
Cardiovascular disease and heart disease are often used interchangeably. While the conditions share many of the same characteristics, the serious ways in which they affect the body can actually be different. Here is a helpful breakdown to help you remember these key terms.
As mentioned above, this catchall refers to all types of diseases of the heart or blood vessels, including clogged arteries (heart disease) which can lead to heart attacks, strokes, and congenital heart defects.
Any condition affecting the heart’s function and structure is heart disease. While heart disease is a type of cardiovascular disease, and thus all heart diseases are also cardiovascular diseases, not all cardiovascular diseases are a form of heart disease.
Heart disease can encompass many different issues which are often related to atherosclerosis, or the formation of plaque along the artery walls. Heart disease can therefore lead to heart attack or stroke.
A stroke occurs when a blood vessel that feeds or is located within the brain becomes blocked or bursts. This starves the brain of blood and oxygen, causing brain cells to die. If too many brain cells die, the effects of a stroke can be permanent, but in cases where enough brain cells survive, injured cells can be repaired and impaired functions may improve.
While understanding the key differences among these conditions is important, cardiovascular diseases as a whole share many of the same causes, risk factors, early warning signs, and prevention tactics. Because of this, and the fact that heart disease and stroke are so closely related, we will focus on the characteristics of heart disease for the remainder of this guide.
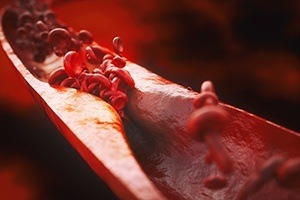
Atherosclerosis is the most common cause of heart disease.[2] As the plaque thickens along artery walls, it causes the walls to stiffen, which can prevent blood from flowing freely through your arteries to your vital organs and tissues.
Alarmingly, the signs of atherosclerosis may never be outwardly visible – that is, until a plaque ruptures or builds up to the point where blood flow is completely restricted. If you have atherosclerosis in your heart valves, you may develop symptoms such as angina (chest pain). The appearance of this symptom calls for quick action, however, as it often precedes a heart attack. [3]
The plaque development which characterizes atherosclerosis develops slowly over time. While the exact cause of the condition is unknown, experts strongly believe it can result from many different factors, such as:
While atherosclerosis is the most common cause of heart disease, it isn’t the only one. Heart arrhythmias (abnormal heart rhythms), congenital heart defects, cardiomyopathy (thickening of the heart muscle), and heart infections can also lead to heart disease. Arrhythmias are caused by many of the same factors as atherosclerosis including high blood pressure, tobacco use, and smoking, but can also be brought on by excessive caffeine or alcohol use, illicit drug use, and stress.
In addition to the primary causes, there are many behaviors and other risk factors which can contribute to your likelihood of developing heart disease.
Common risk factors associated with heart disease include:
Age plays an important role in raising the risk of heart disease. In men, the risk for heart disease begins to increase at the age of 45. For women, the age is 55. [5] While age-related behavioral factors, such as poor nutrition and sedentary lifestyles, can contribute to heart disease risk, biological changes also factor in. For instance, the blood vessels naturally become less flexible as we age, which makes it more difficult for blood to pass through.
For many years, heart disease was perceived to be commonly seen in men. Now, however, it has been established that it is the leading cause of death for both sexes. After the age of 65, men and women share roughly the same risk. With that said, the symptoms of heart disease in diabetic women tend to be less obvious than in their male peers. For example, women may only experience shortness of breath during physical activity, versus men who experience chest pain.[6]
Your blood pressure measures the force of your blood pressing against your blood vessel walls. Having high blood pressure creates added stress on your heart and blood vessels causing them to work harder. High blood pressure also creates friction, which damages the tissues in your arteries, causing bad cholesterol to develop within the tears in the artery walls and prompting atherosclerosis.
Unhealthy blood cholesterol levels increase heart disease risk in the ways outlined above. Poor diet is one of the main culprits behind high cholesterol.
Saturated fats, commonly found in animal products, can raise your cholesterol levels. In particular, red meat and full-fat dairy could lead to increased cholesterol, but this is oftentimes a result of poor selection of raw materials. For example, grass-fed beef is leaner than grain-fed beef, and both meat and dairy from hormone-free sources are considered healthiest. Of course, genetic factors should be assessed to create a meal plan to support each patient’s unique needs. If an individual’s genetics do not make them susceptible to cholesterol increases, full-fat dairy and red meat typically needn’t be restricted.
On the other hand, commercially baked cookies, crackers, and other processed foods are problematic in that they often contain cholesterol-raising trans fat, and even when they don’t, they can contribute to inflammation, a common culprit behind chronic illness and a suspected causative agent behind heart disease.
In diabetes, the body fails to produce ample insulin or cannot use insulin properly, causing blood sugar levels to spike. Over time, this increased level of blood glucose can damage your blood vessels, along with the nerves controlling your heart. Adults with diabetes face twice the risk of fatal heart disease or stroke compared to those without.[7]
Limiting poor-quality carbohydrates that have a significant impact on insulin response is critically important to preventing insulin resistance, and subsequently, the development of type 2 diabetes.
It is carbohydrates – and in particular, high-glycemic-index carbohydrates – which most substantially increase cardiovascular-related disease by modulating insulin and inflammation and causing a negative impact on the cardiovascular system.
High-glycemic index foods, including white bread, rice, and processed snacks such as breakfast cereals and packaged cakes or cookies, pose an especially concerning threat for patients with excess body fat and exercise limitations. Diets rich in these foods could place an individual at risk for diseases related to inflammation, including heart disease, especially when coupled with a sedentary lifestyle.
Adults have a significantly increased risk of developing any form of cardiovascular disease if they are overweight or obese. Specifically, obese or overweight adults between the ages of 40 and 59 have an increased risk ranging from 21-85%, compared to normal-weight peers.[8]
The relationship between heart disease and being overweight is complex, but most notably, carrying extra weight creates a ripple effect of damage on the heart as it is associated with hidden inflammation which can impede your heart’s ability to function properly.
Smoking damages and constricts blood vessels, and has also been found to raise cholesterol and blood pressure levels. Moreover, it can prevent ample oxygen from reaching the body’s critical organs and tissues, thereby increasing heart disease risk.[9]
Genetics can play a major role in determining risk factors for cardiovascular disease. Unfortunately, most individuals are unaware of specific testing that is available to establish a better understanding of individual risks. For example, Apolipoprotein E (ApoE) is a protein found in your blood that carries cholesterol and triglycerides to the liver, where they are removed from the blood and also impacts additional enzymatic functions that aid in the removal of these lipids.
There are 6 possible genotypes with 2 genotypes carrying a high risk for developing heart disease, 2 carrying intermediate-risk, and 2 carrying normal risk. [10] Those with the highest risk genotype experience a 40X greater risk of developing cardiovascular disease than their normal risk counterparts. Not only does knowing your genotype determine your potential risk factors, but it also provides insight as to how effective clinical interventions with medication and lifestyle modifications can be.
Another inherited risk factor is familial hypercholesterolemia (FH) – a defect that affects how the body recycles low-density lipoprotein (LDL) or “bad” cholesterol. The result is very high LDL levels, above 190mg/dL, and is known to be caused by a mutation in the gene for the LDL cholesterol receptor. According to the results from the 1999-2012 National Health and Nutrition Examination Survey, roughly 1 in 250 adults have the FH genetic mutation. [11]

A sedentary lifestyle is a major cause of chronic diseases, including heart disease. Studies have even indicated that the increase in risk associated with reduced fitness is comparable to or greater than other clinical factors, such as smoking and diabetes.[12]
Exercise contributes to cardiovascular health in numerous ways. It controls blood pressure, increases “good” HDL cholesterol, improves circulation to prevent clots which can lead to heart attack and stroke, and aids in weight regulation
Research shows up to 44% of people with heart disease also have major depression, and individuals hospitalized for heart attack are about three times as likely to have depression. While individuals with heart disease often face stress related to health issues, depression itself also appears to be a risk factor for heart disease. While the precise interplay is still unclear, experts believe both inflammatory and lifestyle changes related to depression can impact cardiovascular health.[13]
While calculating your risk for all cardiovascular issues, including heart disease and stroke, is an important foundational step in preventing a deadly cardiac event, it’s also critical to watch for the early signs of heart disease. Identify what to look for in the next section.
Frustratingly, many of the early signs of heart disease mimic those seen in other health issues. Further, some of these symptoms are even ignored as signs of aging or inactivity. Yet, when they are intense or appear out of the blue, it’s worth taking note. Patients should always be mindful of any unfamiliar developments in their health and err on the side of caution because by the time signs of a heart attack manifest it is likely past the point of prevention.
Early signs of heart disease can include unexplained aches or pain. When the blood supply to the heart is blocked, it can cause significant strain and, subsequently, pain in the heart. Yet, this pain isn’t always experienced in the chest. It can also be felt in the arms, shoulders, back, or even the jaw or abdomen. Symptoms that occur with activity but fade with rest are especially important to note, as they can indicate heart issues.
Shortness of breath is another telling sign of heart problems. While it’s possible for anyone to become winded after exertion, climbing just a few stairs shouldn’t leave you out of breath. Extreme shortness of breath, accompanied by pressure or pain in the chest, dizziness or lightheadedness, extreme fatigue, pain in the regions described above, or extreme fatigue could indicate a heart attack, which demands immediate medical attention.
Additionally, heart palpitations, characterized by irregular or rapid beating, can signify heart issues. While they are often harmless and can occur with anxiety, caffeine, and dehydration, unexplained palpitations occurring while at rest should be investigated by a physician. Note how often they occur and what you’re doing when they happen.
Being mindful of these signs, along with your individual risk factors, can be helpful in preventing heart disease. With that said, the most comprehensive approach to prevention should incorporate the expertise of physicians who employ the next generation of medicine to stop heart disease before it even starts.

There are many preventive tactics within your reach, which you can begin implementing right away. Smoking cessation, diet and weight management, exercise, and blood pressure and cholesterol control are among the most powerful lifestyle changes you can make to prevent heart disease.
Yet, a key component of prevention is knowing your individualized risk for heart disease and stroke. Metrics such as blood pressure levels can only tell you so much, and without insights garnered from more advanced, comprehensive laboratory screenings, we only see a small portion of overall heart disease risk.
With its innovative Heart Disease & Stroke Prevention Program, Cenegenics provides life-saving testing, going beyond conventional screening to assess in-depth genetic factors, advanced lipid panels, laboratory markers for plaque formations, and assessments for inflammatory markers which contribute to cardiovascular disease.
By combining the expertise of three cardio-diagnostic leaders and implementing aspects from the nation’s two top laboratories screening for cardiovascular disease, we have developed an industry-leading program to provide the most specific and accurate cardiac health picture currently available.
The findings retrieved from your screenings allow our physicians to offer patient-focused, specific recommendations based on your unique needs. From providing nutritional adjustments such as sodium intake and nutraceuticals to tailoring exercise plans to encourage physical fitness that is both effective in reducing disease risks and safe for your current abilities, our clinical team takes an all-encompassing approach to not only supporting your heart health but also your overall wellness.
And, because our experts remain at the forefront of age management medicine, all of our programs are tailored to accommodate age-related risk factors and concerns, thereby allowing you to minimize the risk of deadly disease and feel great through every decade of life.
If you’re interested in preventing heart disease, stroke, and other chronic illnesses while becoming the healthiest possible version of yourself, contact a Cenegenics location near you.
Our world-class physicians create a personalized plan to help you feel 10+ years younger. You’ll be more energetic, lose weight, sleep better, have more libido, and think more clearly. Visit our website for more information, as well as to book your free consultation.
 Contributor: Rudy Inaba Vice President of Health Performance
Contributor: Rudy Inaba Vice President of Health Performance
Rudy Inaba is Cenegenics’ Vice President of Health Performance. He is a recognized fitness and sports nutrition consultant with nearly 15 years of experience in clinical exercise physiology and lifestyle management. After pursuing his Master of Science in Clinical Exercise Physiology at the University of Nevada Las Vegas, Rudy joined Cenegenics where he leads 19 clinical locations nationwide in their advancements in kinesiology, nutritional biochemistry, and their analyses of industry research & market trending.


