
I’m at the point where food has taken
the place of sex in my life.
Rodney Dangerfield
As we age, the hormones in our body undergo changes. While the decrease in hormone levels experienced by women in their middle ages, known as menopause, has been a well-known characteristic of aging for many years, men’s age-related hormone changes have only been studied in depth within recent decades. The purpose of this research has been to answer the question: Do men, too, experience menopause?
While the condition isn’t exactly akin to menopause, men do indeed experience development of symptoms resulting from a decrease in the male hormone testosterone. This condition is referred to as andropause, a set of symptoms directly related to decreases in testosterone levels that occur with age. It affects up to 30% of men in their 50s and becomes more prevalent with age.[1]
We’ve compiled this guide to help you better understand andropause and make informed decisions about your health. Discover some information about the condition including its symptoms, how it’s diagnosed, and available treatments below.
While changing hormone levels are a natural part of aging, when symptoms begin to interfere with an individual’s quality of life, it becomes necessary to look into suboptimal testosterone. Diagnosed low testosterone can have a strong or heightened influence on age-related symptoms. Indeed, age is a major influencing factor in testosterone levels, but weight is also correlated with testosterone deficiency rates. For each decade of life, the prevalence of testosterone deficiency increases by 17% after the third decade, but an increase of body mass index of 4-5 is also associated with an increased prevalence of 17% every decade. Thus, although testosterone does decline naturally with age, poor nutrition and exercise can also exacerbate or spur symptoms of andropause.
With that said, testosterone deficiencies are by no means rare. While the reported prevalence of testosterone deficiency varies significantly, ranging from 2.1% to 39% of men aged 40 and older, the Hypogonadism in Males (HIM) Study suggests as many as 13.8 million men aged 45 and older in the U.S. alone could be biochemically testosterone deficient.
Yet, if low testosterone, and thus andropause, are such widespread issues, why aren’t more men receiving treatment? Both this and the wide range in reported prevalence can be attributed to the fact that there is a lack of consensus on what, specifically, defines testosterone deficiency. For this reason, it’s important to understand the ways in which andropause can be diagnosed.
One of the primary challenges in measuring testosterone is that the ways in which the body uses the hormone are complex. While a man can have levels of total testosterone that are clinically defined as being “normal,” only some of that is available for use by the body, or “free” testosterone. Men experiencing andropause tend to have lower levels of free testosterone, and the tissues in the body stimulated by testosterone receive lower amounts. This can lead to a variety of physical and mental symptoms.
The questions surrounding how best to measure testosterone are further complicated by the fact that hormone levels can vary based on a number of factors, including:
Simply put, measuring testosterone alone does not truly reflect the clinical effect of the entire androgen system. For this reason, age management specialists use both total and free testosterone measurements alongside several other hormone-related blood tests and clinical assessments to diagnose andropause. While clinical criteria are less specific, they are of equal or greater priority in making an accurate diagnosis.
To perform a clinical assessment, physicians discuss with their patients the symptoms that accompany testosterone deficiency in three domains: physical, sexual, and emotional.
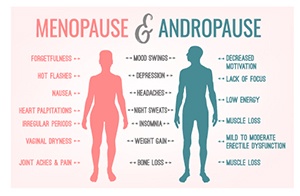
The symptoms of declining testosterone levels can vary significantly from one person to the next. While each individual may experience them differently, the most common symptoms of andropause include:
Other common symptoms of andropause can be grouped into the following domains: physical, sexual, and emotional.
The most common symptoms of andropause within the physical domain are:
Commonly reported sexual symptoms of andropause to include:
In the emotional realm, the most common symptoms experienced are:
Unfortunately, despite its host of unpleasant symptoms, andropause goes untreated far too often. There is a widespread notion that because sex hormone deficiency is a natural part of aging, no correction is required. Yet, this challenging set of symptoms can impact men in their social, professional, and personal lives, eventually taking their toll and leading to an overall decline in physical and mental health.
Moreover, if the physical, sexual, and emotional symptoms aren’t compelling reasons enough to seek treatment, consider this: testosterone deficiency leads to:
It is therefore recommended that any man who suspects he could be experiencing the symptoms of andropause seek the professional opinion of an experienced age management specialist. There are many treatments available for testosterone deficiency, which brings us to our next section.

Factors such as age and general health status must always be accounted for when treating andropause. With that said, hormone replacement therapy has been shown to benefit young, elderly, healthy, and unhealthy men. Oftentimes, the most significant improvements are seen in the sexual domain.
When coupled with sound nutrition and exercise, however, hormone replacement therapy becomes a powerful treatment with benefits transcending into the physical and emotional domain, too. Improved muscle strength, physical function, lean body mass, and mood are just some of the positive changes that targeted treatment can achieve.
It’s important to emphasize, however, that treatments must always be based on an individual needs analysis. Age management specialists will discuss a number of treatment strategies regarding the use of bioidentical hormones, but these must be carefully considered by both the physician and the patient. Moreover, individualized dietary changes and exercise plans should be provided if the goal is to improve overall vitality, not just improvements in the sexual domain.
Because the symptoms of andropause are unique to each patient, and each patient likewise has their own individual set of preexisting health factors to consider, it’s critical for men to work with experienced age management professionals when seeking treatment for low testosterone. More importantly, comprehensive monitoring must be performed to ensure the patient’s progress is aligning with treatment goals and that biomarkers are within appropriate values.
Cenegenics age management specialists take an all-encompassing approach to treating andropause. Our team dynamically shifts nutrition and exercise goals and efforts, as needed, based on how patients respond and adapt and continuously monitor the impact of bioidentical hormones through comprehensive lab work. Our physicians are experts in the distinct needs of adults approaching their middle ages and beyond and are committed to helping them achieve a better quality of life and future, in which the symptoms of andropause and other age-related conditions are avoided or minimized.
If you’re interested in exploring andropause treatments, contact your nearest Cenegenics location today.
Our world-class physicians create a personalized plan to help you feel 10+ years younger. You’ll be more energetic, lose weight, sleep better, have more libido, and think more clearly. Visit our website for more information, as well as to book your free consultation.
 Contributor: Rudy Inaba Vice President of Health Performance
Contributor: Rudy Inaba Vice President of Health Performance
Rudy Inaba is Cenegenics’ Vice President of Health Performance. He is a recognized fitness and sports nutrition consultant with nearly 15 years of experience in clinical exercise physiology and lifestyle management. After pursuing his Master of Science in Clinical Exercise Physiology at the University of Nevada Las Vegas, Rudy joined Cenegenics where he leads 19 clinical locations nationwide in their advancements in kinesiology, nutritional biochemistry, and their analyses of industry research & market trending.


